If your joints ache for no apparent reason, your hormones–not your age–might be the real culprit. Millions of adults suffer from chronic joint pain that cannot be explained by injury or overuse alone. Recent research 1 suggests that hormone imbalances, especially estrogen, may silently drive joint degeneration by affecting cartilage repair, inflammation, and muscle strength. Women aged 45-64 are three times as likely to have radiographic knee osteoarthritis. Understanding this hormonal link provides a new, evidence-based path to long-term relief.
Are you tired of living with constant joint pain that limits your energy, mood, and mobility? At Vita Bella, we believe true healing starts from within by restoring balance to your body’s natural hormones. Discover how optimizing estrogen, testosterone, and cortisol can transform your joint health, reduce pain, and renew your energy. Keep reading to learn the science-backed connection between hormone balance and pain-free living and how you can start your journey to stronger, healthier joints today.
Is Estrogen the Body’s Natural Joint Repair Crew for Women?
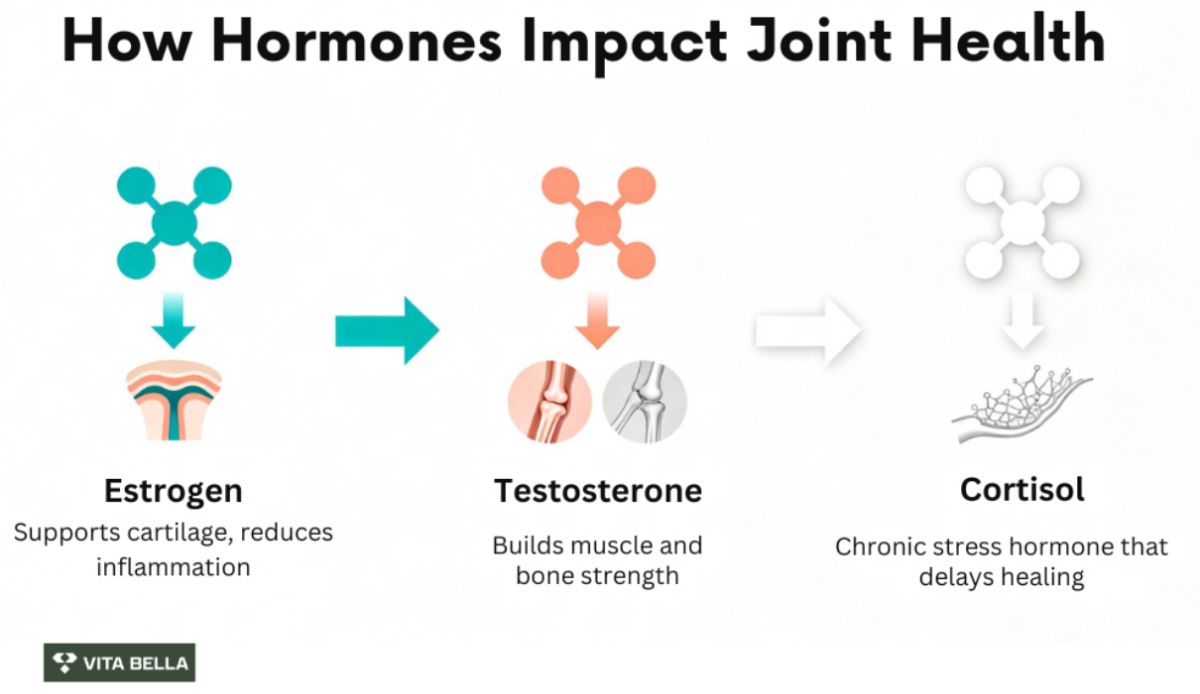
Estrogen is one of the most protective hormones for joint tissue. It helps maintain cartilage, reduce inflammation, and preserve subchondral bone density. After menopause, estrogen levels drop significantly, and the risk of osteoarthritis (OA) rises significantly. Researchers 1 note that “the steep increase in OA prevalence after menopause suggests estrogen deficiency accelerates disease progression”.
A 2023 study 2 found that perimenopausal women with lower estrogen levels had more severe knee pain and greater cartilage degradation, driven by increased inflammatory cytokines. Women undergo a variety of physiological and psychological changes as they approach the perimenopausal stage, mainly as a result of notable variations in estrogen levels. Estrogen also appears to promote collagen synthesis in joint tissue, explaining why its decline leads to joint stiffness and inflammation.
Another study 3 showed that post-menopausal women develop more rapid cartilage thinning and subchondral bone remodeling than pre-menopausal women, changes that predict early OA. This structural degeneration often manifests as morning stiffness and joint swelling. For women approaching menopause, evaluating estrogen balance through blood tests can provide early warning signs. Discussing bioidentical or transdermal estrogen therapy with a clinician may help protect joint integrity and reduce OA risk when clinically appropriate.
Is Testosterone Essential for Building Muscle Mass, Supporting Bone Health, and Promoting Tissue Healing?
Testosterone acts as a stabilizer for the musculoskeletal system. It maintains lean muscle mass and bone density, two vital components that protect and align the joints. According to research 4, as men age, testosterone levels typically decline by about 2% per year after age 40, leading to muscle loss (sarcopenia) and reduced mechanical support for joints.
A systematic review 5 of randomized trials found that testosterone replacement therapy (TRT) increased muscle strength with a standardized mean difference of 0.21 (95% CI 0.15–0.28) in older men with low testosterone. Greater muscle strength directly improves joint stability and reduces mechanical stress. Oral testosterone supplementation was given at 160 mg/day in one study.
Is Cortisol the Hidden Factor that Blocks Your Body’s Natural Healing Process During Stress?
Cortisol, the body’s primary stress hormone, is essential in short bursts but harmful when chronically elevated. Persistently high cortisol suppresses immune cells, slows tissue regeneration, and increases inflammatory cytokines. In the context of joint pain, this means slower repair of cartilage and connective tissue, resulting in chronic stiffness and swelling.
A 2024 review 6 highlighted how long-term activation of the hypothalamic-pituitary-adrenal (HPA) axis elevates cortisol, leading to “substantial immunosuppressive effects on immune cells,” ultimately blunting the healing response. Patients with elevated cortisol also exhibit elevated C-reactive protein (CRP), a marker of systemic inflammation linked to joint pain.
Can an Integrative, Hormone-based Approach Effectively Reduce Chronic Joint Pain and Improve Mobility?
An integrative, hormone-based approach may help alleviate joint pain by addressing underlying hormonal imbalances that affect inflammation, cartilage repair, and tissue regeneration. Balancing hormones such as estrogen, testosterone, and cortisol can enhance joint flexibility, reduce stiffness, and promote long-term mobility. Combining hormone optimization with lifestyle modifications offers the most comprehensive solution for chronic joint discomfort. Clinicians recommend:
Screening for estrogen, testosterone, and cortisol imbalances in adults with persistent or unexplained joint pain.
Optimizing muscle and bone strength via resistance training and adequate dietary protein.
Consider hormone therapy in consultation with specialists when imbalances are clinically confirmed.
Reducing stress through meditation, yoga, or breathwork to modulate cortisol and inflammation.
Monitoring results using objective markers, joint function tests, bone density scans, and hormone panels.
Heal from Within, Targeted Solutions for Lasting Relief with Vita Bella.
Painkillers may mask the ache, but they don’t fix the real issue. Hormonal shifts silently weaken cartilage and muscle, leaving your joints unprotected. Whether it’s post-menopause or age-related testosterone decline, the result is the same: persistent pain and slow recovery. As hormones decline, your body’s ability to repair tissue and maintain muscle support around joints dramatically weakens.
At Vita Bella, we target the hormonal root of joint pain. Our experts combine medical insights, nutrition, and lifestyle programs to rebalance your hormones and regenerate joint strength from within. Through advanced testosterone optimization and guided hormone therapy, we help restore lean muscle, stabilize joints, and enhance healing naturally. Start your healing journey where it truly begins inside your body, with the right balance of hormones supporting every move.

FAQs
Can a hormone imbalance really cause chronic joint pain?
Yes. Hormone imbalance can significantly contribute to chronic joint pain by disrupting cartilage repair, bone density, and the control of inflammation. Low estrogen after menopause accelerates osteoarthritis, while low testosterone reduces muscle support around joints. Elevated cortisol from chronic stress further hinders tissue healing, compounding pain and stiffness over time.
Does restoring hormonal balance help reduce joint pain naturally?
Yes. Correcting hormonal imbalance through medical evaluation, lifestyle changes, and, when appropriate, hormone therapy can improve joint comfort and mobility. Balanced estrogen supports cartilage health, testosterone restores muscle strength, and cortisol regulation enhances healing. Addressing these factors holistically can reduce inflammation, slow degeneration, and promote long-term joint resilience.
Should both men and women get their hormone levels tested for joint pain?
Yes. Both men and women benefit from hormone testing when facing unexplained or chronic joint pain. Women may experience estrogen drops after menopause, while men often lose testosterone with age. Identifying these shifts early allows for personalized interventions that protect cartilage, enhance muscle function, and restore overall joint health.
Can lifestyle changes balance hormones and ease joint pain?
Yes. Regular strength training, stress management, and nutrient-rich diets help regulate hormones naturally. Exercise boosts testosterone and estrogen sensitivity, while mindfulness and quality sleep lower cortisol. Combined, these habits reduce inflammation and strengthen muscles around joints, creating a robust foundation for long-term pain relief and joint protection.
References:
Atasoy-Zeybek, A., Showel, K. K., Nagelli, C. V., Westendorf, J. J., & Evans, C. H. (2025). The intersection of aging and estrogen in osteoarthritis. npj Women’s Health, 3(1), 15. https://doi.org/10.1038/s44294-025-00063-1
Zhao, H., Yu, F., & Wu, W. (2025). The mechanism by which estrogen level affects knee osteoarthritis pain in perimenopause and non-pharmacological measures. International Journal of Molecular Sciences, 26(6), 2391. https://doi.org/10.3390/ijms26062391
Castañeda, S., & Vicente-Rabaneda, E. F. (2023). Disentangling the molecular interplays between subchondral bone and articular cartilage in estrogen deficiency-induced osteoarthritis. Osteoarthritis and Cartilage, 31(1), 6-8. https://doi.org/10.1016/j.joca.2022.09.006
Grossmann, M., Anawalt, B. D., & Yeap, B. B. (2024). Testosterone therapy in older men: Clinical implications of recent landmark trials. European Journal of Endocrinology, 191(1), R22–R31. https://doi.org/10.1093/ejendo/lvae071
Lee, T.-W., Kao, P.-Y., Chen, Y.-C., & Wang, S.-T. (2023). Effects of testosterone replacement therapy on muscle strength in older men with low to low-normal testosterone levels: A systematic review and meta-analysis. Gerontology, 69(10), 1157–1166. https://doi.org/10.1159/000532062
Balakin, E., Yurku, K., Ivanov, M., Izotov, A., Nakhod, V., & Pustovoyt, V. (2025). Regulation of stress-induced immunosuppression in the context of neuroendocrine, cytokine, and cellular processes. Biology, 14(1), 76. https://doi.org/10.3390/biology14010076